New Study Claims Med Diet Reduces Heart Disease Risk By 25%
Updated March 21st 2023

Women who follow the principles of The Mediterranean Diet can reduce their risk of Cardiovascular Disease and death by nearly 25%, according to new research.
Contents:
- Study links reduced risk of heart disease in women with Mediterranean Diet
- Extra Virgin Olive Oil And The Mediterranean Diet
- Mediterranean Diet Prevents Repeat Heart Attacks And Strokes
- Benefits of Extra Virgin Olive Oil, Fatty Fish, and Nuts For Your Heart
- Morocco Gold Extra Virgin Olive Oil For Cardiovascular Health
- Improve Your Health Using A Premium Extra Vigin Olive Oil
The study, which was carried out by the University of Sydney in Australia and reported in the BMJ, explored links between diet and cardiovascular disease, which accounts for more than a third of all deaths in women worldwide.
Researchers analysed previous research and clinical trials that looked at the impact of eating a Mediterranean diet – known for including extra virgin olive oil as a healthy fat – on women’s health. The studies involved more than 700,000 women whose cardiovascular health was monitored for an average of 12.5 years, according to a news release.
The study found that strict adherence to a Mediterranean diet was associated with a 24% lower risk of cardiovascular disease among women, and a 23% lower risk of mortality from any cause.
“This study supports a beneficial effect of the Mediterranean diet on primary prevention of CVD and death in women, and is an important step in enabling sex specific guidelines,” the authors wrote.
Extra Virgin Olive Oil And The Mediterranean Diet
The Mediterranean Diet has been proven to significantly reduce the risk of heart disease. The Mediterranean Diet is high in fiber, fruits, vegetables, legumes, and extra virgin olive oil.
Mediterranean-style cooking consists of ingredients that are naturally rich in monounsaturated fats, which are beneficial for long-term health. Extra Virgin Olive Oil is also packed full of antioxidants to prevent cellular damage in the body.
Mediterranean Diet Prevents Repeat Heart Attacks And Strokes
The Mediterranean Diet could be the best choice for patients with established coronary heart disease, according to a new study published in The Lancet.
According to the research, monitoring over 1,000 cardiovascular patients for seven years, the rate of recurrence in those on the Mediterranean diet was between 25% and 30% lower than normal.
Dr López Miranda, who led the research, said the study showed that in patients with coronary disease, the Mediterranean diet has a greater effect on preventing recurrence than the low-fat diet, and Dr Delgado Lista, of the University of Cordoba, agreed that the results were of major significance for everyday clinical practice.
The Mediterranean Diet is known for its reliance on healthy monounsaturated or polyunsaturated fats, primarily sourced from extra virgin olive oil.
As reported by SurinEnglish, lifestyle is a major factor in preventing the occurrence and recurrence of cardiovascular events, combined with medication and other procedures.
In a further report on the survey by tctmd.com, the latest CORDIOPREV is the only trial in the past 23 years which compares the Mediterranean diet against another eating pattern for secondary prevention.
“To our knowledge, this study is the most extensive to date evaluating the effects of a Mediterranean diet and a low-fat diet in the prevention of recurrent cardiovascular events in the context of two high-intensity dietary interventions,” write Javier Delgado-Lista, MD (Hospital Universitario Reina Sofia, Córdoba, Spain), and colleagues May 4, 2022, in the Lancet.
It follows the landmark PREDIMED study, which was first published in 2013, established the Mediterranean diet for the primary prevention of major cardiovascular events.
Benefits of Extra Virgin Olive Oil, Fatty Fish, and Nuts For Your Heart

For the Mediterranean diet, participants consumed 35% of their calories from fat, mostly monounsaturated (22%) and polyunsaturated fat (6%). Protein made up 15% of the diet and the remaining calories were comprised of carbohydrates (< 50%). The diet included 40 to 60 g of extra-virgin olive oil, three or more servings of especially fatty fish per week, and three or more servings of nuts per week, among other foods. Wine was optional, but if participants were habitual wine drinkers, it was capped at one to two glasses per day for women and men, respectively.
For the low-fat diet, less than 30% of calories were derived from fat, 15% from protein, and 55% or more from complex carbohydrates. Participants ate low-fat dairy two or three times per day and chose lean fish instead of fatty kinds. Nuts were limited, as was EVOO. Instead, the intervention recommended only 20 to 30 g of sunflower or regular olive oil. Wine was not allowed.
No physical activity was prescribed, nor was any type of caloric restriction. To make sure patients adhered to the diet, they had face-to-face visits with dieticians, internists, or cardiologists every 6 months, group sessions every 3 months, and telephone calls every 2 months. In total, participants had at least 12 interactions with the study team each year.
After 7 years of follow-up, there were 198 primary outcome events: 17.3% in the Mediterranean arm and 22.2% in the low-fat group. In the unadjusted and adjusted models, the Mediterranean diet was associated with a significantly lower risk of the primary endpoint. Adjusted for age and sex alone, eating the diet rich in EVOO, fatty fish, and nuts was associated with a 26.2% lower risk of the primary outcome (P = 0.034). In the fully adjusted model, the Mediterranean diet lowered the risk of the primary outcome by 28.1% compared with the low-fat diet (P = 0.024). The was no significant difference in the risk of any of the primary endpoint’s individual components.
In 2021, the American Heart Association (AHA) issued new lifestyle and dietary recommendations that focus on dietary patterns as opposed to individual foods or nutrients. They recommend people eat mostly plants for protein but also fish and seafood. While the AHA doesn’t explicitly push the Mediterranean diet, they do say that this diet can help people achieve healthy dietary patterns.
Morocco Gold Extra Virgin Olive Oil For Cardiovascular Health
Olive oil may help lower the risk of heart disease, according to preliminary research that also showed it was beneficial as a substitute for butter or mayonnaise.
“Previous studies have linked high consumption of olive oil with better cardiovascular health, particularly in Mediterranean countries where olive oil intake is much higher than in the United States,” lead study author Marta Guasch-Ferre said in a news release.
“Our aim was to investigate whether higher olive oil consumption was beneficial to heart health in the U.S. population,” said Guasch-Ferre, a research scientist in the department of nutrition at Harvard T.H. Chan School of Public Health in Boston.
The study, presented Thursday at the American Heart Association’s Epidemiology and Prevention/Lifestyle and Cardiometabolic Health Scientific Sessions, examined 63,867 women and 35,512 men from 1990 to 2014. All participants were free of cancer, heart disease and other chronic diseases at the start of the study. Every four years, they answered questionnaires about their diet and lifestyle.
Researchers found those who ate more than half a tablespoon of olive oil each day had a 15% lower risk of having any kind of cardiovascular disease and a 21% lower risk of coronary heart disease. Replacing one teaspoon of butter, margarine, mayonnaise or dairy fat with the same amount of olive oil lowered the risk of cardiovascular disease by 5% and coronary heart disease by 7%. However, consuming more olive oil didn’t impact stroke risk.
Although olive oil proved to be healthier than butter and margarine, it did not present more benefits than other plant oils like corn, canola, safflower and soybean.
“One interesting thing our study shows is that although olive oil was better than most animal fats and margarine, it was not superior to vegetable oils in this study population,” Guasch-Ferre said. “This means that replacing any type of animal fat with vegetable oils, including olive oil but also others, could be a good strategy to improve cardiovascular health.”
Researchers noted many margarines contained substantial amounts of trans fatty acids when the study began in 1990, so the results may not apply to vegetable margarines now available.
The findings were observational, which means they don’t prove cause-and-effect. However, small intervention studies have found replacing animal fats with olive oil has a beneficial effect on fat levels in the blood.
“Future research is needed to investigate the mechanisms behind this association as well as the effects of other vegetable oils on heart health”
Marta Guasch-Ferre
The results, also published in the Journal of the American College of Cardiology, provide further reason to incorporate more plant-based foods into our daily diets, said nutrition expert Penny Kris-Etherton.
“Using vegetable oils in cooking and in salads makes good sense,” Kris-Etherton said in a news release. She is a distinguished professor of nutrition at Pennsylvania State University and chair of the AHA’s Lifestyle and Cardiometabolic Health Council. “Research has overwhelmingly found that diets that are rich in plant-based foods, including healthier vegetable oils such as olive, safflower, corn and many others, can significantly benefit heart health,” she said.
Olive Oil Consumption and Cardiovascular Risk in U.S. Adults
Background:
Olive oil intake has been associated with lower risk of cardiovascular disease (CVD) in Mediterranean populations, but little is known about these associations in the U.S population.
Objectives:
This study sought to examine whether olive oil intake is associated with total CVD, coronary heart disease (CHD), and stroke risk.

Methods:
This study included 61,181 women from the Nurses’ Health Study (1990 to 2014) and 31,797 men from the Health Professionals Follow-up Study (1990 to 2014) who were free of cancer, heart disease, and stroke at baseline. Diet was assessed using food frequency questionnaires at baseline and then every 4 years. Cox proportional hazards regressions were used to estimate hazard ratios (HRs) and 95% confidence intervals (CIs).
Results:
During 24 years of follow-up, this study documented 9,797 incident cases of CVD, including 6,034 CHD cases and 3,802 stroke cases. After adjusting for major diet and lifestyle factors, compared with nonconsumers, those with higher olive oil intake (>0.5 tablespoon/day or >7 g/day) had 14% lower risk of CVD (pooled HR: 0.86; 95% CI: 0.79 to 0.94) and 18% lower risk of CHD (pooled HR: 0.82; 95% CI: 0.73 to 0.91). No significant associations were observed for total or ischemic stroke. Replacing 5 g/day of margarine, butter, mayonnaise, or dairy fat with the equivalent amount of olive oil was associated with 5% to 7% lower risk of total CVD and CHD. No significant associations were observed when olive oil was compared with other plant oils combined. In a subset of participants, higher olive oil intake was associated with lower levels of circulating inflammatory biomarkers and a better lipid profile.
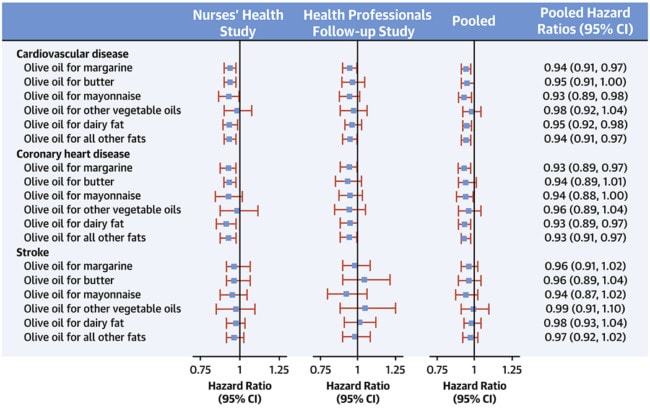
Conclusions:
Higher olive oil intake was associated with lower risk of CHD and total CVD in 2 large prospective cohorts of U.S. men and women. The substitution of margarine, butter, mayonnaise, and dairy fat with olive oil could lead to lower risk of CHD and CVD.
Keywords:
Cardiovascular disease; coronary heart disease; olive oil; plant oils; stroke.
Source: Heart.org