Why A Quality Extra Virgin Olive Oil Can Help You Tackle LDL Cholesterol
Updated December 16th 2022
Summary
- High cholesterol is when you have too much of a fatty substance called cholesterol in your blood.
- There are two types of molecules called lipoproteins that carry cholesterol in the blood: low-density lipoprotein (LDL) and high-density lipoprotein (HDL).
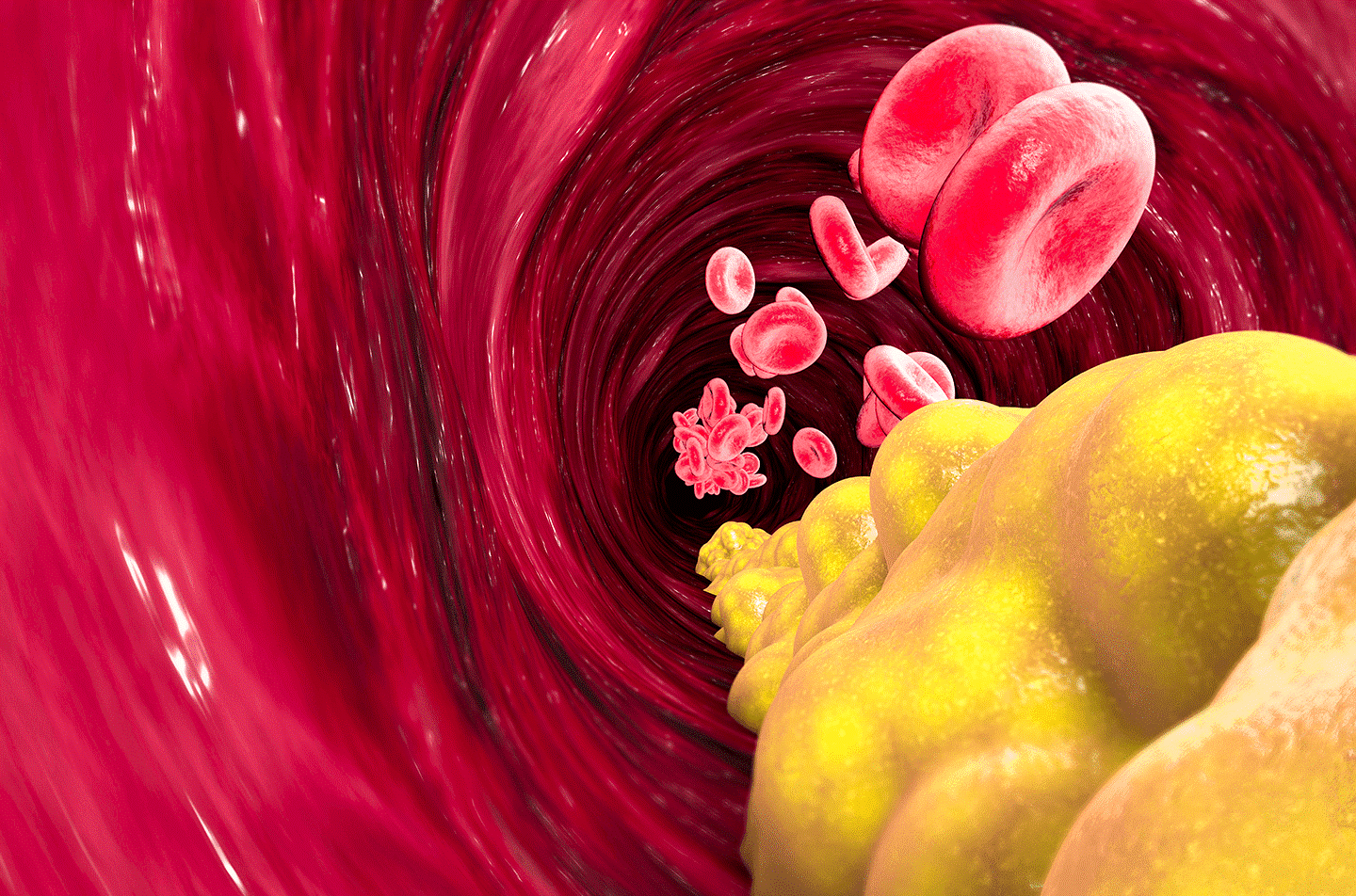
- LDL is known as “bad” cholesterol, since having high levels of LDL can bring about plaque build-up in the arteries, which can result in heart disease and stroke.
- HDL is known as “good” cholesterol; HDL (good) absorbs cholesterol and carries it to the liver where it is flushed from the body.
- Two landmark clinical trials, one employing a cholesterol-lowering statin drug and reported a 30% mortality reduction, the second utilizing the Mediterranean diet and reported a 70% mortality reduction.
- In clinical studies, improved HDL (good) function was more pronounced for participants taking a Mediterranean diet enriched with extra virgin olive oil.
Contents
- Extra Virgin Olive Oil And LDL Cholesterol
- Olive Oil: Why Choose It Over Other Saturated Fats?
- What is High Cholesterol?
- Can The Mediterranean Diet Help Reduce LDL Cholesterol?
- The Health Benefits Of Extra Virgin Olive Oil : A Further Study
Extra Virgin Olive Oil And LDL Cholesterol
Olive oil can help reduce cholesterol. If you are looking to decrease levels of LDL (bad) cholesterol in your arteries and arm yourself against heart disease, including a quality olive oil in your diet is a great place to start. By substituting saturated fats for healthier unsaturated fats and polyunsaturated fats (both present in extra virgin olive oil) you are contributing to a reduced risk of the health complications caused by high levels of LDL (bad) cholesterol.
Olive Oil: Why Choose It Over Other Saturated Fats?
By making a change from saturated fats, such as butter, lard or animal fats to extra virgin olive oil, which contains much higher levels of monounsaturated or polyunsaturated fats, you are helping to reduce the risk of high cholesterol affecting the function of your heart and arteries.
What is High Cholesterol?
High cholesterol is when you have too much of a fatty substance called cholesterol in your blood. It is mainly caused by eating fatty food, not exercising enough, being overweight, smoking and drinking alcohol. It can also run in families. You can lower your cholesterol by eating healthily and getting more exercise. Some people also need to take medicine. Too much cholesterol can block your blood vessels. It makes you more likely to have heart problems or a stroke. High cholesterol does not cause symptoms. You can only find out if you have it from a blood test.
Cholesterol travels through the blood on proteins called “lipoproteins.” Two types of lipoproteins carry cholesterol throughout the body:
LDL (low-density lipoprotein), sometimes called “bad” cholesterol,makes up most of your body’s cholesterol. High levels of LDL cholesterol raise your risk for heart disease and stroke.
HDL (high-density lipoprotein), or “good” cholesterol,absorbs cholesterol and carries it back to the liver. The liver then flushes it from the body. High levels of HDL cholesterol can lower your risk for heart disease and stroke.
Can The Mediterranean Diet Help Reduce LDL Cholesterol?

Nearly twenty years ago two landmark randomized clinical trials appeared in The Lancet which forever changed the course of medicine for patients with coronary heart disease (CHD). The 4S study employed a cholesterol-lowering statin drug and reported a 30% mortality reduction. The Lyon Diet Heart Study utilized the Mediterranean diet and reported a 70% mortality reduction.
Subsequent studies of the Mediterranean diet have confirmed these findings and have also shown a reduced risk of cancer, diabetes, and Alzheimer’s disease. Subsequent statin studies have led the United States Food and Drug Administration to issue warnings regarding the increased risk of diabetes and decreased cognition with statin drugs. Paradoxically, statins have gone on to become a multi-billion dollar industry and the foundation of many cardiovascular disease prevention guidelines while the Mediterranean diet has often been ignored.
The authors of the study, Robert DuBroff and Michel de Lorgeril concluded “we believe this statin-centric cholesterol-lowering approach to preventing CHD may be misguided”. They further found.
The dramatic benefits of the Mediterranean diet are likely due to multiple mechanisms which do not directly involve cholesterol. Independent of cholesterol metabolism are the true fatal complications of coronary atherosclerosis – thrombotic coronary occlusion, acute myocardial ischemia, left ventricular dysfunction, and malignant arrhythmias.
The hemostatic system appears to be a principal modulator of atherosclerotic plaque formation and progression and the Mediterranean diet can favourably alter elements of the coagulation cascade. Plaque rupture and intra-plaque haemorrhage leads to progressive atherosclerosis, thrombosis causes acute coronary syndromes, and sudden cardiac death is the main cause of cardiac mortality.
At the genetic level large scale, genome-wide association studies have identified 46 loci directly linked to CHD, yet a majority of these loci have no apparent relation to cholesterol or traditional risk factors. Although we can’t change our genes, epigenetic studies have shown that the Mediterranean diet can favourably alter the expression of atherogenic genes, whereas a recent cholesterol-lowering statin trial failed to demonstrate a similar effect.
Source: WJC
The Health Benefits Of Extra Virgin Olive Oil : A Further Study
Montserrat Fitó, Ph.D., is the senior author of research by the Cardiovascular Risk and Nutrition Research Group at the Hospital del Mar Medical Research Institute in Barcelona, Spain. Fitó and team’s findings were published in the American Heart Association’s journal Circulation.
There are two types of molecules called lipoproteins that carry cholesterol in the blood: low-density lipoprotein (LDL) and high-density lipoprotein (HDL).
LDL is known as “bad” cholesterol, since having high levels of LDL can bring about plaque build-up in the arteries, which can result in heart disease and stroke. HDL is known as “good” cholesterol; HDL (good) absorbs cholesterol and carries it to the liver where it is flushed from the body. Having high levels of HDL (good) reduces heart disease and stroke.
The research team aimed to determine whether eating a Mediterranean diet enriched with extra virgin olive oil or nuts over a long period of time would improve the beneficial properties of HDL (good) cholesterol in humans.
Fitó and collaborators randomly selected a total of 296 individuals who had a high risk of heart disease and were participating in the Prevención con Dieta Mediterránea study. The participants had an average age of 66 and were assigned to one of three diets for a year.
The first diet was a traditional Mediterranean diet enriched with around 4 tablespoons of extra virgin olive oil per day. The second, a traditional Mediterranean diet supplemented with a fistful of nuts each day. The third diet was a healthful “control” diet that contained a reduced amount of red meat, high-fat dairy products, processed foods, and sweets.
Both Mediterranean diets emphasized the inclusion of fruit, vegetables, legumes (such as beans, chickpeas, lentils, and whole grains), and moderate amounts of fish and poultry.
Blood tests were conducted at the start and end of the study to measure LDL (bad) and HDL (good) levels.
Extra Virgin olive oil-enriched Mediterranean diet enhanced HDL function
The researchers found that total and LDL (bad) cholesterol levels were only reduced in the healthful control diet. While none of the three diets significantly increased HDL (good) levels, the two Mediterranean diets improved HDL (good) function, and the improvement was more pronounced in the group enriched with extra virgin olive oil.
The Mediterranean diet enriched with extra virgin olive oil improved HDL (good) functions, such as reversing cholesterol transport, providing antioxidant protection, and enabling vasodilation.
Reverse cholesterol transport is the process in which HDL (good) removes it from plaque in the arteries and takes it to the liver. Antioxidant protection is the ability of HDL (good) to counteract the oxidation of LDL (bad). Oxidation of LDL (bad) triggers the development of plaque in the arteries.
Lastly, vasodilator capacity, which relaxes the blood vessels, keeps them open, and keeps the blood flowing, is improved by the Mediterranean diet with extra virgin olive oil.
Although the control diet was rich in fruits and vegetables like the two Mediterranean diets, the diet was shown to have an adverse impact on HDL’s (good) anti-inflammatory properties. This negative impact was not observed in the Mediterranean diets. A reduction in HDL’s (good) anti-inflammatory capacity is linked with a greater risk of heart disease.
“Following a Mediterranean diet rich in virgin olive oil could protect our cardiovascular health in several ways, including making our ‘good cholesterol’ work in a more complete way.”
Montserrat Fitó
Source: https://www.medicalnewstoday.com/articles/315818.php?bl
Note : Readers with concerns over Cholesterol levels should consult their doctor